Chronic diabetic ulcers remain one of the most stubborn and devastating complications of diabetes, and many patients face years of pain as poor circulation and chronic inflammation prevent wounds from closing. More than 40 million people in the United States live with diabetes, and diabetic foot ulcers are a leading cause of amputation, affecting nearly one third of patients with severe wounds. Existing treatments rely heavily on biological materials taken from pigs or human cadaver skin, but these options come with serious drawbacks. Pig derived products can trigger immune reactions, while human donor tissues are limited in supply and often come from older donors with reduced regenerative capacity. Variability among donors can also lead to inconsistent healing and poor mechanical matching with the patient’s own tissue.
Researchers at Texas A&M University are developing a new approach that avoids these limitations by turning human cells into manufacturers of regenerative materials. Instead of transplanting donor cells or animal derived tissues, the team guides laboratory grown human cells to build an interwoven extracellular matrix that mimics the structure of healthy skin. Once the matrix is produced, the cells are removed, leaving behind a biological scaffold that is human derived, consistent in quality, and free from the risks associated with living donor cells. Because the material originates from engineered human cells, it can be produced in unlimited quantities and does not carry the pathogen or rejection risks associated with animal products.
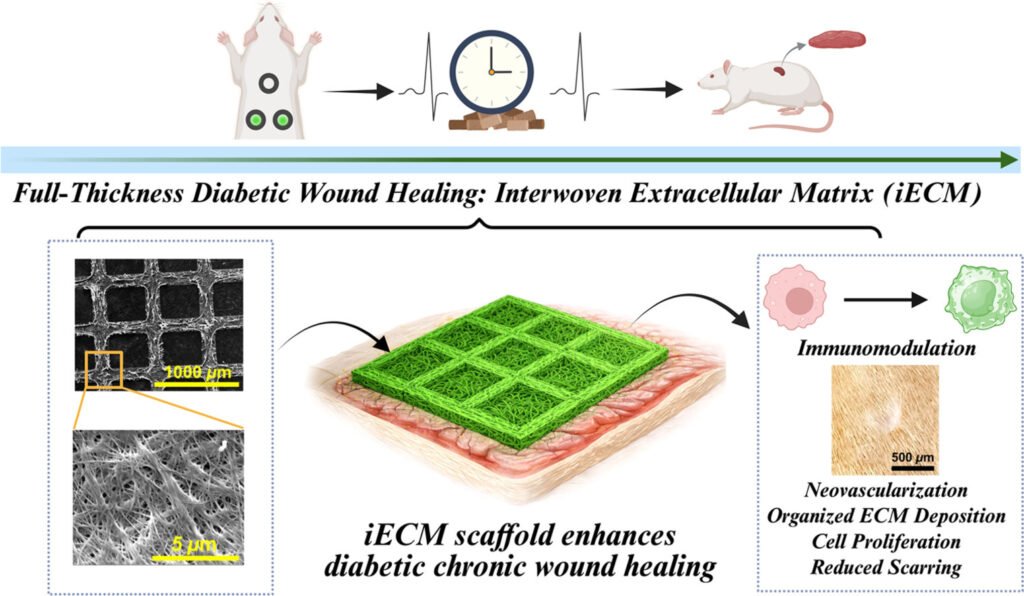
The researchers describe the process as giving cells a framework and letting them build the house. By providing a structural guide, they can coax cells to assemble the same complex architecture found in natural skin. This interwoven extracellular matrix is designed to support healing by reducing inflammation, encouraging the formation of new capillaries, and avoiding the immune complications that often slow recovery in diabetic wounds. Early laboratory images show immune cells shifting from inflammatory behavior to healing behavior after the matrix is applied, suggesting that the material may help redirect the wound environment toward regeneration. If successful, this approach could offer a more reliable and regenerative option for patients with diabetic ulcers, reducing the need for amputations and improving long term healing outcomes.
Article from Texas A&M: Novel diabetic wound treatment turns cells into manufacturers
Abstract in Acta Biomaterialia: Human cell-derived dermal-specific interwoven extracellular matrix for diabetic wound healing