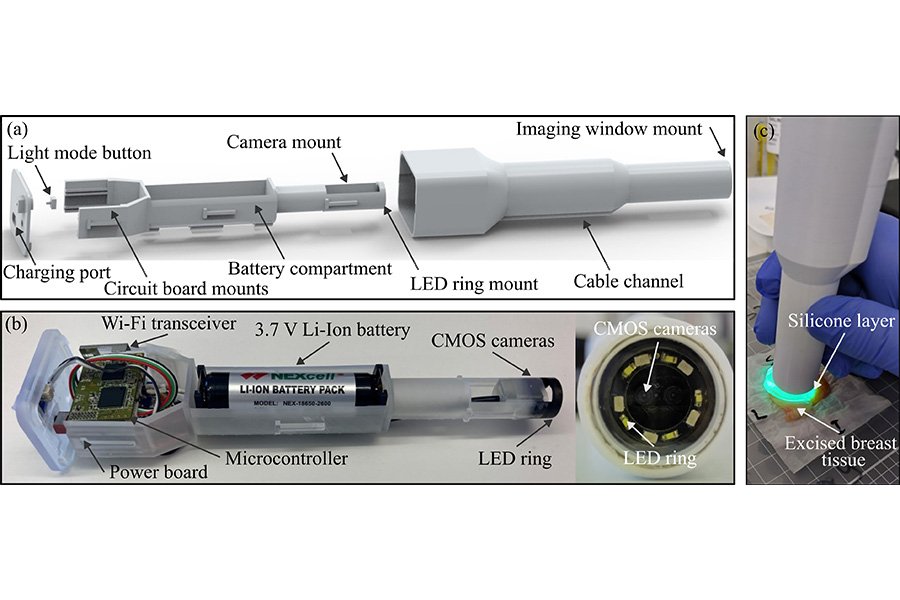
Cancer surgeons often struggle to distinguish healthy tissue from malignant tissue during an operation, and this uncertainty can lead to incomplete tumor removal or unnecessary damage to surrounding structures. A team of researchers has developed a handheld optical probe that addresses this long standing challenge by mapping cancerous tissue in real time. Their device gives surgeons immediate feedback about the biochemical makeup of tissue, allowing them to make more confident decisions while operating.
The technology is built around a technique called Raman spectroscopy, which uses light to detect the molecular composition of a sample. When the probe shines a laser onto tissue, the light scatters in patterns that reveal the presence of specific biomolecules. Cancer cells have distinct molecular signatures compared with healthy cells, and the probe interprets these signatures instantly. This approach eliminates the delays associated with sending tissue samples to a pathology lab during surgery.
Researchers tested the probe on a range of cancer types, including breast, brain, and skin tumors. In each case, the device was able to differentiate malignant tissue from normal tissue with high accuracy. The team emphasized that the probe does not require dyes, contrast agents, or any additional preparation. It works directly on living tissue, which makes it practical for use in the operating room. Surgeons can move the probe across the surgical field and receive continuous updates about tissue composition, creating a live molecular map of the area they are working on.
One of the most important advantages of the device is its potential to reduce the need for repeat surgeries. When surgeons cannot clearly identify tumor margins, patients may return for additional procedures to remove remaining cancerous tissue. By providing immediate molecular information, the handheld probe helps ensure that surgeons remove the full extent of the tumor during the first operation. This can improve outcomes, shorten recovery times, and reduce emotional and financial burdens on patients.
The research team also highlighted the probe’s portability and ease of use. Because it is compact and handheld, it can be integrated into a wide range of clinical environments, including smaller hospitals that may not have access to advanced imaging systems. The device’s real time capabilities also make it suitable for minimally invasive procedures where visual cues are limited.
By giving surgeons a tool that reveals the molecular landscape of tissue as they operate, this handheld probe represents a significant step toward more precise and personalized cancer surgery. It brings laboratory level analysis directly into the operating room and offers a new way to improve surgical accuracy and patient safety.
Article from AIP: Mapping Cancerous Tissue with a Hand-Held Probe
Abstract in APL Bioengineering: A wireless and handheld optical palpation imaging probe for use in breast-conserving surgery